To develop new treatments for cancer, scientists are focused on finding the malfunctioning machinery within cancer cells that can be targeted using small molecule pharmaceuticals. Now, University of Michigan researchers have identified one of these targets: a zinc and calcium ion permeable channel within a cell’s lysosome, the organelle responsible for recycling cellular waste, nutrient sensing and cell metabolism.
The researchers discovered that this channel is upregulated—meaning both its protein expression and channel activity were substantially increased—in metastatic melanoma cells compared with healthy melanocytes. They found that targeting this channel protein with small pharmaceutical compounds triggers the rapid and selective death of cancer cells while completely sparing normal cells. Their research is published in the journal Cell Reports.
“Many traditional cancer therapies target a well-known cell death pathway called apoptosis to trigger cancer cell death. However, many aggressive cancer cells harbor numerous mutations of genes that help them escape these treatments. We saw an urgent need to develop new therapeutic strategies that target nonapoptotic cell death pathways to eradicate cancer cells,” said Wanlu Du, an assistant research scientist in the U-M Department of Molecular, Cellular, and Developmental Biology.
In metastatic cancers, lysosomes turn hypertrophic, which means they actively contribute to tumor progression by increasing their ability to provide nutrients to the rapidly dividing cells and secreting enzymes to digest extracellular matrix—the material that provides the physical scaffolding for cells to help cancer cell invasion. But designing cancer therapies that target lysosomes may also harm normal cells and tissues by compromising lysosomes’ ability to provide nutrients for healthy cells.
Instead, the U-M researchers focused on specific machinery within lysosomes that are hijacked by cancer: TRPML1. TRPML1 is a protein channel that ferries metal ions, including iron, zinc and calcium, across the lysosome membrane and into the cell.
The researchers examined protein expression levels of TRPML1 in normal skin tissues, benign and metastatic melanoma. In addition, they measured the channel activity by directly patch-clamping the cell’s lysosome. The researchers then examined the effect of pharmacological molecules, called TRPML1 agonists and antagonists, on cancer cells viability.
The research team, led by Du and U-M researcher Haoxing Xu, found that activating, rather than inhibiting, this zinc/calcium ion channel caused cancer cells to die—but did not cause harm in healthy cells.
“This is the first example of an opposite way to think about cancer treatment,” said Xu, senior author of the paper and professor of molecular, cellular, and developmental biology. “Cancer is caused by maladaptation, or upregulation, in many signaling pathways, which results in excessive, uncontrolled cell growth. The traditional anticancer approach is straightforward: to inhibit or decrease maladaptive upregulation.
“We now demonstrated that giving a further boost to the ‘bad,’ cancerous signaling can selectively ‘kill’ the cancer cells.”
To determine what was responsible for the cell death when activating TRPML1, the researchers examined the effect of different metal ions on the cell death. They found that zinc permeability of TRPML1 played a critical role in the process.
“When we tested different ion blockers to see which could prevent the cell death, we found that if we blocked lysosomal zinc release, we could completely block this type of cell death,” Du said. “This is why we believe this channel activation and lysosomal zinc release mediates this kind of cell death.”
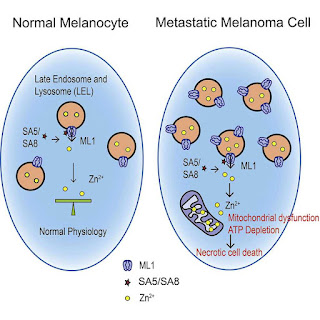
The researchers’ study shed light on a new cell death pathway they call “lysozincrosis”—a combination of lysosome, zinc and necrosis. This pathway is mediated by the activation of TRPML1, lysosomal zinc ion release, and mitochondria dysfunction.
Fellow U-M authors include Mingxue Gu, Meiqin Hu, Prateeksunder Pinchi, Wei Chen, Michael Ryan, Timothy Nold and Ahmed Bannaga.
Source/Credit: University of Michigan
scn102121_02