|
| Associate Professor Ge Ruowen (left) from NUS Biological Sciences and Professor Fred Wong (right) of NUS Pharmacology. Credit: National University of Singapore |
NUS scientists have discovered a novel property of a protein found in human lungs which could lead to the development of biologic drugs to treat chronic obstructive pulmonary disease (COPD), a debilitating, progressive lung disease that is one of the leading causes of death worldwide.
The research was led by Associate Professor Ge Ruowen from NUS Biological Sciences and published in the prestigious scientific journal Proceedings of the National Academy of Sciences.
Fighting COPD
COPD is currently the third-leading cause of death globally and poses a large socioeconomic burden on nations. It can be caused by long-term exposure to irritants or particulate matter, such as cigarette smoke, and symptoms include coughing, breathing difficulties, mucus production and wheezing.
Patients with COPD display two key conditions - emphysema (the destruction of alveolar walls and enlargement of the alveoli) and chronic obstructive bronchitis (inflamed small airways). These patients suffer persistent respiratory symptoms with progressive long-term lung function decline. However, current drugs targeting COPD only provide symptomatic relief and are not able to suppress the underlying tissue inflammation to effectively block the spread of COPD or reduce mortality.
“COPD patients have difficulty breathing which hinders their ability to work or exercise. They do not absorb enough oxygen, and this affects their heart function too. COPD is a very dangerous condition, but public awareness of it is very low,” said Assoc Prof Ge.
Maintaining lung health
Alveolar macrophages (AMs) are immune cells residing in the airspace of lung breathing structures called alveoli and they can display either pro-inflammatory or anti-inflammatory properties. In COPD, the pro-inflammatory AMs are amplified, which is a main cause of COPD.
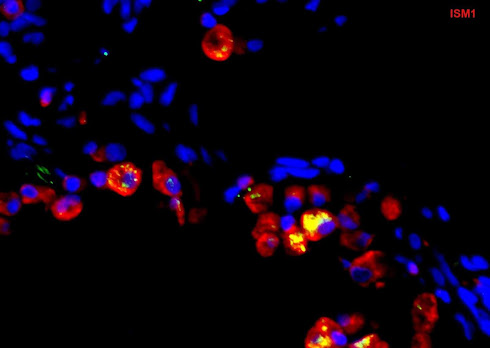
Assoc Prof Ge’s team discovered that a lung-resident protein, called isthmin 1 (ISM1), is critical for restraining inflammation in a healthy lung by selectively eliminating the pro-inflammatory type of AMs. In their laboratory studies, the research team observed that the absence of the ISM1 protein was associated with large numbers of pro-inflammatory AMs, enduring lung inflammation, progressive emphysema and significant lung function decline even without exposure to irritants.
The team discovered that ISM1 helps to maintain healthy lungs by targeting the GRP78 signaling receptor (csGRP78) that is present on the surface of the pro-inflammatory AM, triggering apoptosis (cell death), thereby reducing inflammation.
Developing enduring treatment for COPD
Endogenous – or internal – ISM1 proteins may not be sufficient to counteract lung inflammation in COPD.
To address this challenge, the research team worked with Professor Fred Wong at NUS Pharmacology to conduct laboratory studies to examine the effectiveness of delivering recombinant ISM1 protein directly via droplets into the airway. The researchers observed a reduction in lung inflammation, suppression of emphysema development, and restoration of lung functions. These findings lend support to the development of ISM1 as a potential treatment for COPD.
“By directly targeting pro-inflammatory AMs using recombinant ISM1 protein, our novel treatment suppresses the root cause of COPD, and opens up the possibility of developing this into a viable treatment for this debilitating disease that affects many patients around the world,” said Assoc Prof Ge.
“These findings not only provide a new avenue to develop novel and effective drugs for COPD, but also warrant studies of ISM1 in other inflammatory respiratory diseases,” added Prof Wong.
The development of a drug based on this research is currently in the pre-clinical stages of testing.
Future research
Assoc Prof Ge and her team plan to study how recombinant ISM1 could also help to develop treatments for other inflammatory respiratory disorders such as acute lung injury, lung fibrosis and asthma, and to devise the best method to administer such therapeutics.
Source/Credit: National University of Singapore
med042522_01