 |
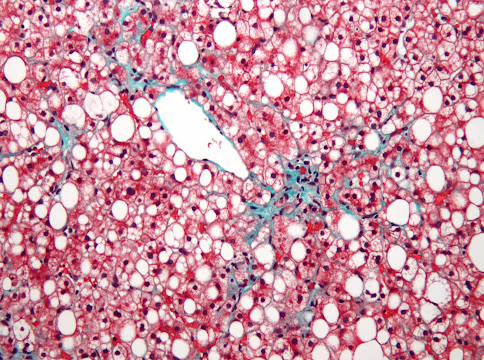
| Micrograph of non-alcoholic fatty liver disease (NAFLD). Masson's trichrome & Verhoeff stain. The liver has a prominent (centrilobular) macrovesicular steatosis (white/clear round/oval spaces) and mild fibrosis (green). The hepatocytes stain red. Macrovesicular steatosis is lipid accumulation that is so large it distorts the cell's nucleus. Image Credit: Nephron CC BY-SA 3.0 |
There is currently no drug for treating non-alcoholic fatty liver disease, which affects many people with type 2 diabetes and which can result in other serious liver diseases. A study led by researchers from Karolinska Institutet has now identified a drug candidate for the treatment of fatty liver. The preclinical study, published in the Journal of Hepatology, indicates that an antibody that blocks the protein VEGF-B presents a possible therapeutic option for fatty liver disease.
“Fatty liver is associated with several serious and sometimes fatal diseases,” says the study’s first author Annelie Falkevall, researcher at the Department of Medical Biochemistry and Biophysics, Karolinska Institutet, Sweden. “With the therapeutic principle that we’ve developed, it might be possible to prevent fatty liver and hopefully lower the risk of liver failure and terminal liver cancer.”
For decades, obesity and overweight have been a common global disease that, amongst other problems, has caused a sharp rise in the incidence of type 2 diabetes. According to the Swedish Diabetes Association, there are 500,000 cases of diabetes in Sweden alone, of which 85 to 90 percent are type 2.
Significant rise in liver cancer risk
.jpg) |
| Annelie Falkevall. Photo Credit: Johannes Frandsen. |
White adipose tissue has a remarkable ability to store energy in the form of lipids, but in the case of chronic obesity, and often type 2 diabetes, it is not enough and the concentration of fatty acids in the blood increases. They are therefore stored elsewhere, including in the liver. Not only does the accumulation of fat in the liver interfere with the secretion of glucose and lead to insulin resistance, but it also increases the danger of permanent damage to one of the body’s most important organs.
NAFLD affects over 100 million adults, and previous research indicates a 17-fold higher risk of liver cancer in people with NAFLD. In people with type 2 diabetes, the incidence of NAFLD is 25 to 29 percent. There are at present no approved drugs for treating NAFLD.
Antibody blocks the release of fatty acids
Researchers at Karolinska Institutet, CIBERDEM and CIBEROBN in Spain, CSL Behring in the U.S., and CSL Innovation in Australia have now studied a new method for limiting the development of fatty liver.
.jpg) |
| Ulf Eriksson. Photo Credit: Stefan Zimmerman. |
“We’ve identified a new method of treating fatty liver disease that involves keeping the fatty acids in the adipose tissue so that they don’t leak out and accumulate in the liver,” says the study’s corresponding author Ulf Eriksson, professor at Department of Medical Biochemistry and Biophysics, Karolinska Institutet. “Our results show that the pharmacological blocking of the VEGB-B signal pathway in mice prevents the accumulation of fat in the liver and reduces the risk of NAFLD.”
The study was conducted on normal and genetically modified mice that received different diets and were treated with the drug candidate. The researchers also studied adipose tissue from 48 patients due to having bariatric surgery. One half of the group had NAFLD, and one half did not. Their results reveal a clear correlation between the level of VEGB-B signaling in white adipose tissue and the presence of NAFLD.
“The next step in taking this exciting drug candidate further is to include it in a clinical development program,” says Professor Eriksson.
Funding: The study was financed by the Swedish Research Council, the Swedish Cancer Society, the Swedish Heart and Lung Foundation, the Swedish Diabetes Foundation, the Novo Nordisk Foundation, EFSD and CSL Ltd. The researchers have received research grants and consultancy fees from CSL Ltd
Published in journal: Journal of Hepatology
Source/Credit: Karolinska Institutet
Reference Number: med020323_01
